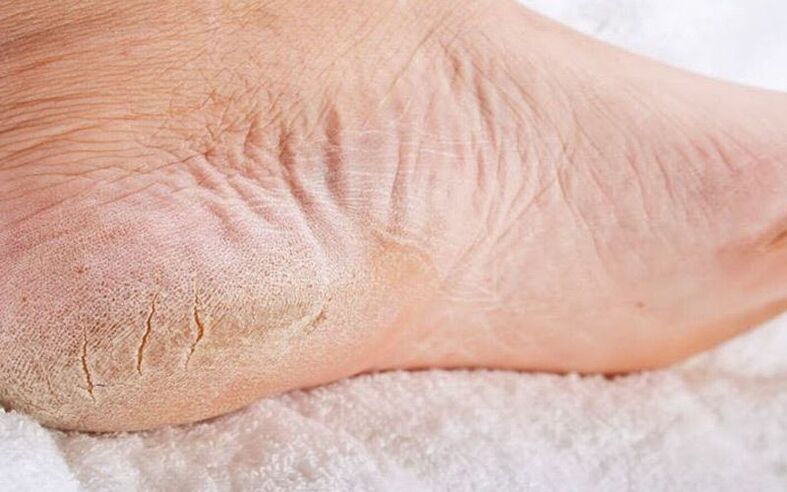
A fungal infection very often affects the toes or nails. This disease affects adults and children. To avoid the pathology becoming chronic, you need to know the signs of foot fungus and what such a disease looks like.
Main signs of the disease
Among all skin diseases, mycosis of the feet is the most common. You can become infected with the disease by ignoring basic hygiene rules. It is sometimes very difficult to cure fungus.
For each person, foot fungus begins and develops in its own way. Here are the most common signs by which foot fungus can be recognized:
- characteristic cracks appear between the toes;
- You can tell that a fungus has appeared by the characteristic itching on your feet and between your toes;
- the skin of the feet is very dry, it often flakes and becomes rough;
- blisters appear between the fingers, which burst when destroyed;
- the infection can spread to neighboring areas;
- reddish spots appear on the skin, which cause significant discomfort;
- You can also recognize foot fungus by its unpleasant smell.
When the first symptoms of the disease appear, you should immediately consult a dermatologist. If you do not do this in advance, it will be much more difficult to treat the fungus.
Signs of fungus depending on the type of pathogen
This disease develops due to different types of pathogens. Symptoms of foot damage will differ in each case.
- If yeast fungus develops on the feet, the nail gradually becomes thinner and peels off from the bed. The skin on the foot is hyperemic (takes on a red tint).
- With the development of epidermophytes, the nail turns yellow and becomes covered with spots. The skin of the feet peels off and gives off an unpleasant odor. A characteristic symptom of this type of fungus is increased dryness of the skin.
- When mold fungus appears, the nail plate can suddenly change its color. The skin turns red if the pathogen gradually spreads to the entire foot. A person is bothered by itching, and the skin may crack. In this case, pain and other unpleasant sensations appear while walking.
Only a doctor can determine the type of pathogen. This cannot be done at home. And if you practice self-medication, you can only harm yourself. Your legs will suffer from this, and the skin fungus will spread more and more.
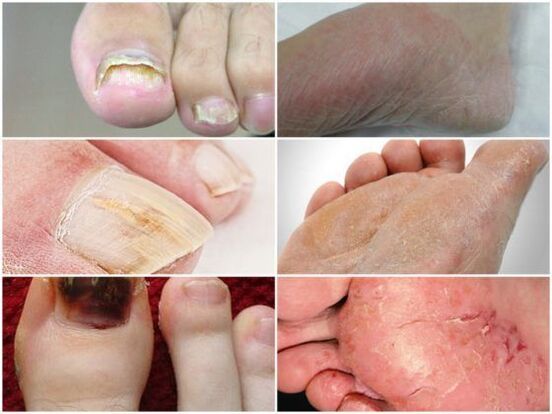
Signs of some forms of fungus
Depending on the affected area and the degree of development, several forms of pathology are distinguished. The symptoms of each are different. Knowing the early signs of foot disease, you can begin treatment for mycosis in a timely manner.
- Interdigital dermatophytosis is the most common stage of the disease. It becomes more active in spring and summer, when feet sweat the most. Cracks and sores appear between the fingers. You can notice the presence of scales on their skin. The foot looks absolutely healthy. Often a person feels itchy.
- The erased form appears to the least pronounced extent. Peeling is noticeable between the fingers. At this stage of the disease, a sharp unpleasant odor spreads from the feet: it appears due to increased bacterial activity.
The disease can occur in various forms. Let's get acquainted with their signs so that we know how to identify fungus on the feet and, if it develops, begin treatment. It must be remembered that in advanced stages of the disease the nail is completely destroyed. It is almost impossible to restore it.
Squamous type
This fungus is characterized by intense peeling of the epidermis. Moreover, it is the areas of skin between the toes and the side of the foot that are most intensively affected. There are no signs of the inflammatory process. In the photo of the first signs of foot fungus, areas of hyperemia are noticeable. Squamous fungus looks like this:
- the stratum corneum thickens;
- the skin shines, sometimes becomes thick;
- the pattern on the skin becomes more distinct;
- the fungus gradually spreads to the fingers, the entire foot, and affects the nails;
- sometimes lamellar scales appear on the epidermis;
- The patient does not feel any other unpleasant sensations.
Dyshidrotic type
With this fungus, small blisters filled with liquid appear on the skin. They are usually found on the side of the foot. Then they gradually move to the inner side of the fingers. How to recognize fungus on the feet of the dyshidrotic type:
- the bubble is usually single, but if there are many of them, they merge into one large one;
- if left untreated, the liquid in the blisters gradually darkens;
- If the blister ruptures, erosion with a crust appears in its place.
With this type of foot fungus, there is a very high risk of bacterial infection. The infection enters the body through open skin lesions.
Intertriginous type
This type of fungus is the most common. At first, the person does not feel any symptoms. Up to a certain point, the skin on the toes does not change. Subsequently, cracks and layers appear. The skin is not affected, but it may sweat.
Candidiasis of the feet
The characteristic symptoms of this fungal infection are as follows:
- the lesion is the 3rd or 4th toe;
- the skin is red and swollen;
- There is a bubble around the lesion where there is a peeled layer of skin;
- There are pustules and blisters nearby.
If a bacterial infection enters the affected area, it leads to an increase in local temperature. Swelling is noticeable on the skin of the legs. In severe cases, a person experiences general hyperthermia.
Signs of fungal nail infection
A person's toenails may also be affected. The disease can be distinguished by the following symptoms.
- Marked change in the color of the nail plate. Depending on what type of pathology the patient has, the nail takes on a variety of shades. Sometimes it can change only on part of the nail plate.
- Nail crumbling. It only happens in advanced stages. If the nail is completely infected, it is destroyed.
- Changes in the structure of the nail.
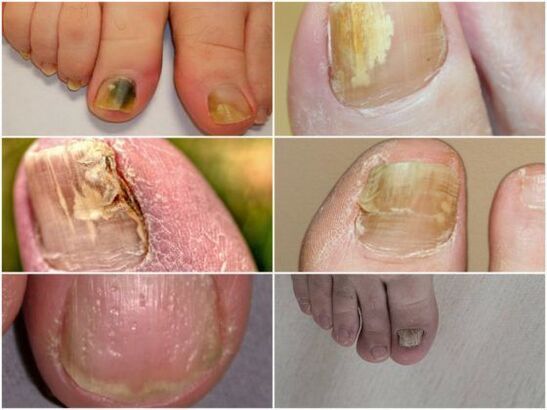
There are several types of onychomycosis, a fungal infection of the nails.
- Atrophic appearance. The nail plate looks very thin. It darkens, sometimes acquiring a grayish-brown color. The nail gradually peels off from its bed. The skin underneath becomes keratinized and becomes loose.
- With the normotrophic form of foot fungus, the plate changes its shade. Spots appear on it - white, yellow, green and even black. The structure of the nail is not affected.
- In the hypertrophic form, the plate gradually thickens and becomes porous. The affected area looks very unsightly and in some cases causes pain while walking. On the sides it crumbles and collapses without treatment.
Some types of onychomycosis
Depending on the degree of spread of the disease, its forms are distinguished.
- Lateral onychomycosis is the most common. A small yellow spot first appears on the free edge of the nail. In the future, you will notice how it increases, and the nail plate thickens. While walking, a person feels discomfort. The spread of an unpleasant odor is noticeable. Lateral onychomycosis is difficult to treat.
- Superficial onychomycosis is characterized by damage to only the upper layers of the plate. It does not thicken, but over time it becomes chalk-like.
- The rarest form of the disease is subungual onychomycosis. The skin thickens noticeably in the nail fold. The nail turns white and loses its transparency.
General principles of treatment
Any treatment of pathology begins with diagnosis. Only then can a suitable remedy be prescribed. Self-medication usually leads to worsening of the condition of the legs. Let's get acquainted with the most common methods of therapy.
- At the first signs of fungal infection, special varnishes, plasters, ointments, and sprays are used. They must be used for a long time and according to the instructions.
- If local therapy is ineffective, complex antifungal drugs are prescribed. They are used orally.
- Surgical removal of the affected nail.
- Laser therapy.
- In advanced forms of the disease, systemic drugs are prescribed.
You can avoid the occurrence of an unpleasant disease by following the rules of hygiene. You should avoid using other people's personal hygiene products (towels, slippers). When the first signs of the disease appear, you should immediately consult a doctor.
Types of mycosis
Fungal infections of the feet usually appear between the toes. It is caused by several types of fungi. This problem is most often inherent in adults, since children's sweat can disarm the fungus.
Mycotic lesions can be of various types:
- candidiasis - occurs when the body's resistance decreases, most often in women;
- epidermophytosis is an exclusively "male" disease that develops due to excessive sweating;
- Rubromycosis is a highly contagious form that can occur even in young children.
Signs and forms of the disease
Signs of fungal infection may vary depending on the age of the patient, the state of the immune system and the nature of the blood circulation.
In a person with a strong immune system, the fungus can remain on the skin for several months without showing itself. Slight itching and slight redness of the skin may occur.
Treatment and best remedies

Advanced mycosis is treated with fungicidal tablets and antimycotic ointments. The latter are used after washing and drying the feet.
Folk remedies are recommended to be used only at the initial stage of the disease, as well as to relieve itching. They must be used with extreme caution as some rely on cauterization of the skin and may cause burns.
As for traditional medicine, they are used at the patient’s own risk. Particular care should be taken when using formulations containing vinegar, celandine or manganese, as this can cause skin burns.
In parallel with drug treatment, you can use baths with oak bark, chamomile or sage. A soda bath effectively reduces itching.
Preventive measures
Although there are effective and inexpensive treatments for foot fungus on the market, it is best not to let the problem develop. Prevention of fungal infection consists of:
- in daily hygiene;
- wearing individual shoes (especially in public showers, baths and swimming pools);
- regularly treating the inside of shoes with ammonia;
- daily change of socks;
- strengthening and maintaining immunity.
These are basic, simple measures that anyone can do. But if infection does occur, then to prevent relapse, it is necessary to treat foot fungus with medications for another 14 days after the complete disappearance of all symptoms of mycosis.
Foot fungus: symptoms and treatment, photo of foot fungus
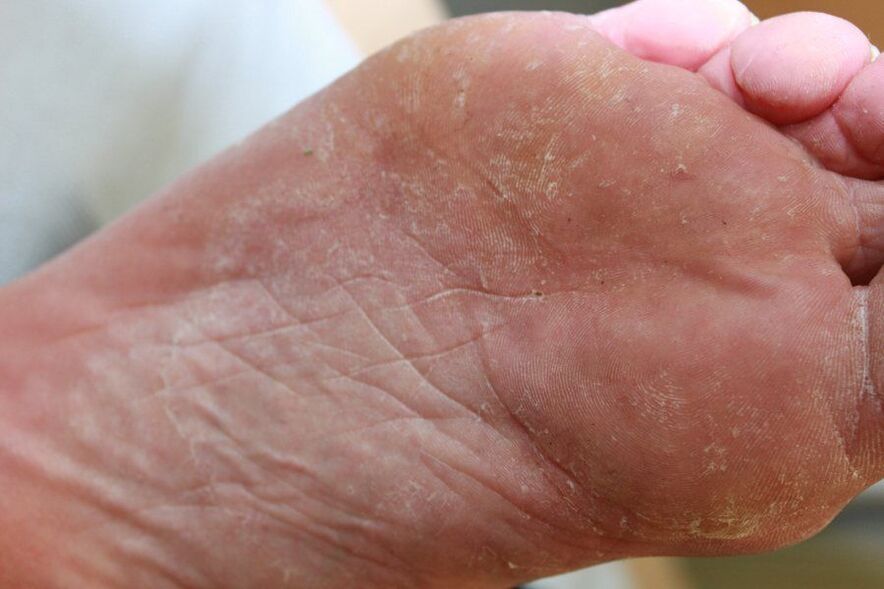
Foot fungus is one of the most common diseases in dermatological practice. It occurs primarily in cultures where it is customary to wear shoes most of the time, and affects up to 70% of the adult population.
Most often, foot fungus is observed in the elderly, as well as those whose immunity is significantly weakened, for example, with diabetes, AIDS, circulatory disorders of the lower extremities and other diseases of this type.
Often, the term "fungus or mycosis of the foot" refers to damage by fungal mycelium to the plantar skin of the feet, nails and interdigital spaces.
Pathogens
Among the numerous types of fungi, the main causative agents of mycosis of the feet are the following:
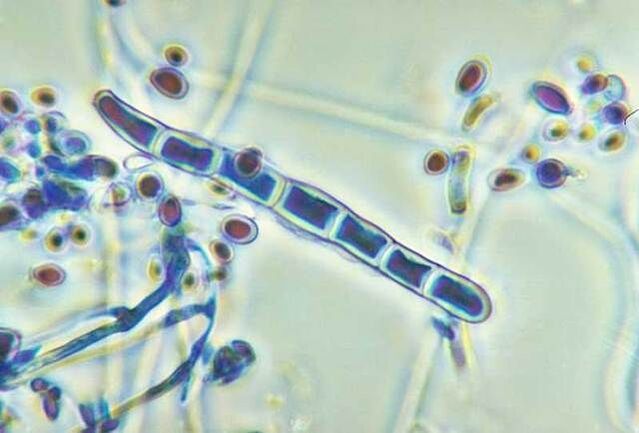
- Trichophyton rubrum,
- Trichophyton mentagrophytes,
- Epidermophyton floccosum.
Other causative agents of fungal infections of the feet, which are not so common:
- Trichophyton tonsurans is the causative agent of mycosis in children in America,
- Candida,
- Scytalidium hyalinum,
- Scytalidium dimidiatum.
All pathogens of fungal infections have adapted to parasitize in the stratum corneum of the skin, producing special enzymes that break down keratin. In addition, their membranes (cell walls) contain manans - special substances that suppress local immunity and contribute to the development of chronic inflammation.
Routes of infection and factors contributing to the disease
It is believed that some types of fungal foot pathogens are capable of maintaining their viability in exfoliated skin flakes for a year. To become infected with a fungus, it is enough for such skin flakes with the pathogen to stick to the legs, and then fall into conditions suitable for reproduction: humidity and heat.
The most common infections with foot fungus occur:
- In public places: baths, beach beds, swimming pools, saunas, even just beach sand.
- In the family: shared house shoes, lack of individual towels for feet, low level of hygiene.
- Habits: exchanging shoes, socks, wearing someone else's shoes (for example, house slippers of the hosts when visiting).
Factors contributing to infection:
- A decrease in local protective forces as a result of circulatory disorders (for example, with vasculitis, obliterating atherosclerosis of the lower extremities), certain chronic diseases (HIV, other immunodeficiency states, diabetes mellitus, etc. ).
- Prolonged sweating of the feet in athletes during long workouts, in the summer when wearing closed or poorly ventilated shoes.
- Cracks and macerations on the skin of the feet.
In general, men get sick more often than women; with age, the frequency of fungal infections of the feet increases. The risk group for fungal infections of the feet are:
- miners,
- military personnel,
- bath attendants,
- regulars of baths and saunas,
- athletes.
Types of disease
According to the location of the pathological focus of the skin on the foot affected by the fungus:
- Interdigital mycosis (dermatophytosis). It is most often observed in the form of chronic (squamous) or acute (intertriginous) forms.
- Plantar mycosis. Most often it manifests itself as peeling and keratinization of the skin of the foot.
- Dyshidrotic dermatophytosis. Bubbles and vesicles form on the skin of the foot, often reminiscent of allergic dermatitis.
- Deep mycosis. In this case, not only the superficial but also the deep layers of the skin are affected.
- Onychomycosis. Toenail fungus infection.
Depending on the type of pathogen, the main fungal diseases of the feet are:
- Athlete's disease caused by Trichophyton mcntagrophytes.
- Rubrophytosis, caused by Trichophyton rubrum.
Rubrophytosis of the feet: main types and symptoms
Rubrophytosis is the most common fungal foot disease. Occurs in almost 70-90% of cases.
Symptoms
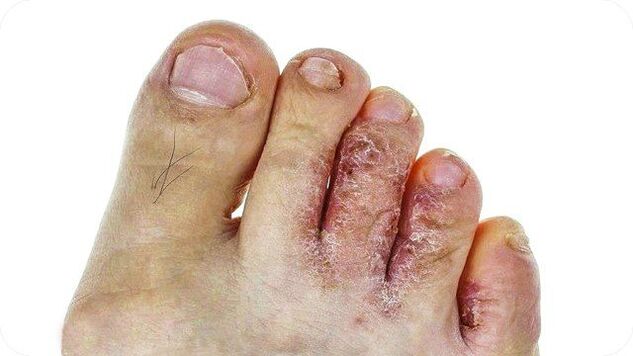
The classic form of rubrophytosis is characterized by redness and moderate thickening (lichenification) of the skin. The affected skin is shiny, with an enhanced pattern, a dry surface with flour-like scales accumulated in the area of grooves and folds.
Usually the disease begins with the third or fourth interdigital fold, which are the tightest. The fungus then spreads to other spaces between the toes, the plantar part and the back of the foot.
The following forms are characteristic of rubrophytia:
Frequently encountered:
- squamous form (the main symptom is flaky skin),
- keratinizing form - the presence of "corns", thickenings.
- intertriginous (opreloid),
- dyshidrotic (with the formation of blisters),
- mixed form (diaper rash, blisters).
On the foot
Erased squamous rubrophytia has the least pronounced symptoms and proceeds almost unnoticed by the patient. Its main symptoms:
- Interdigital spaces: peeling, presence of flour-like scales, superficial small cracks.
- There are practically no complaints or minor itching may bother you.
In this form, rubrophytosis can last for quite a long time. However, the progression of the disease is gradually observed, which leads to the appearance of hyperkeratotic and mixed forms. Gradually there are:
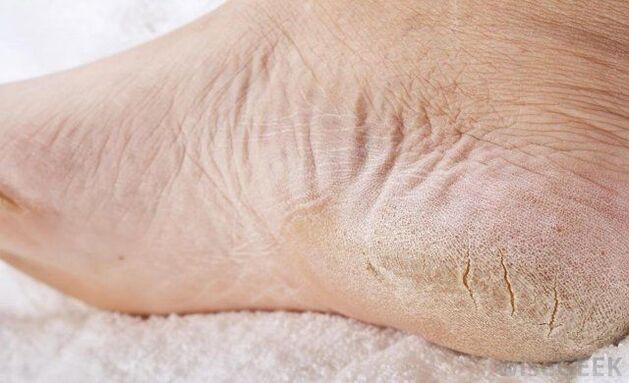
- increased dryness of the skin of the feet,
- roughening of the skin,
- the appearance of rough calluses on the sole and lateral areas of the foot,
- formation of deep and painful cracks in the heel area.
With rubrophytosis of the feet, 3 main types of skin peeling are observed:
- Flourous.The natural folds and furrows of the skin seem to be sprinkled with flour.
- Ring-shaped. Reddened spots with a fringe of exfoliated epithelium.
- Large-lamellar. In this case, the skin peels off in large plates.
In the interdigital spaces
During intense sweating of the feet, wearing poorly ventilated shoes, or inadequate treatment, the spaces between the toes periodically begin to get wet. The skin becomes swollen, eroded, with deep cracks. The main complaints of patients at this stage are itching, soreness, burning.
Without timely and effective treatment, the process gradually worsens, which is manifested by increased pain and itching, which intensify with movement. Large blisters appear on the skin of the interdigital spaces and lateral surfaces of the fingers, which then turn into erosions, surrounded by a border of whitish epidermis.
On the nails
Nail plates of the toes with rubrophytosis:
- thickened,
- crumbling,
- yellowish-gray or with a brown tint,
- chiseled white spots that subsequently spread to the entire nail.
Sometimes they separate from the nail bed, thicken and take on the appearance of a bird's claw or ingrown nail, which causes additional discomfort for patients.
Complications of rubrophytosis
As a rule, rubrophytia spreads to other parts of the body: hands, smooth skin, vellus hair. The pathogen enters new areas of the skin by lymphogenous, as well as contact (for example, transferred by hands when washing feet).
- Hands - damage to the palms and nails.
- Smooth skin - lesions on the face, inguinal-femoral folds, buttocks, legs.
In this case, mycosis manifests itself as round pink-red or pink spots with a tendency to merge and grow peripherally. Their surface is covered with scales, and along the edges there is an inflammatory ridge with small bubbles and crusts.
If rubrophytia has spread to large folds, itching occurs.
Athlete's foot: types and symptoms
Athlete's foot occurs much less frequently than rubrophytosis and has the same forms of the disease:
- Erased.
- keratinizing.
- Diaper rash.
- With the formation of bubbles.
- Athlete's nails.
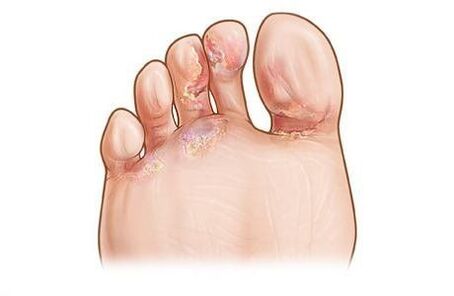
Next, plaque-like thickenings of bluish-red skin appear on the lateral surfaces and sole of the foot. In the center of the rash there are layers of scales, the boundaries of the lesions are clear. In the spaces between the fingers, the epidermis acquires a whitish tint.
With athlete's foot, patients are bothered by itching, increased dryness and soreness of the skin.
The opreloid (intertriginous) form of epidermophytosis is characterized by redness, swelling and maceration of the interdigital folds. Cracks often form and pain is felt.
When the pathogen affects the arch of the foot, a dyshidrotic form can often be observed with the formation of blisters, which, after opening, look like wet erosions of pink or red color.
Athlete's foot most often occurs on the big toe (I) and little toe (V). In the thickness of the nail, closer to the free edge, yellowish spots and stripes form, which gradually increase and occupy the entire nail. Next, the nail begins to crumble, sometimes peeling off from the nail bed.
Acute epidermophytosis Podvysotskaya
The main symptoms of this form of athlete's foot:
- swelling of the feet, fingers,
- abundance of vesicles,
- weeping erosions,
- maceration of interdigital folds,
- enlarged inguinal lymph nodes,
- increase in body temperature,
- headache,
- difficulty walking due to pain,
- general weakness.
Onychomycosis of the toes: symptoms and types
In addition to the causative agents of rubrophytosis and epidermophytosis, onychomycosis can be caused by yeast fungi of the genus Candida, as well as some other fungi.
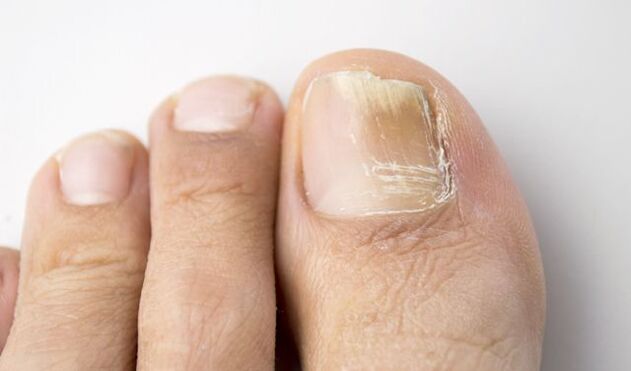
The most typical symptoms of onychomycosis, which begin closer to the free edge of the nail:
- discoloration, loss of natural shine,
- thickening of the nail plate,
- the occurrence of subungual hyperkeratosis,
- destruction of the nail, detachment from the nail bed.
With onychomycosis, there are 2 main types of nail damage:
- Normotrophic: stripes of white and yellowish color are visible in the thickness of the nail.
- Atrophic: thinning, destruction of the nail plate, its detachment.
Diagnosis of fungal infections of the feet
A specialist in the treatment of fungal infections of the feet is a dermatologist who, if necessary, can involve other specialists in treatment.
After a conversation with the patient, clarification of complaints and features of the occurrence and course of the disease, the doctor will examine the affected surface and prescribe some types of additional examination, for example:
- Microscopic examination with additional treatment of the material with potassium hydroxide.
- Wood's lamp examination.
- Inoculation of suspicious biological material on special media for the growth of fungi, as well as on media for bacteria.
Treatment
Treatment for any fungal infection of the feet must be prescribed by a doctor in order to achieve a complete cure.
In general, treatment of foot mycoses is based on the following principles of therapy:
- Fighting the infectious agent. In the initial stages of the disease, local drugs are usually prescribed - antifungal ointments, creams, lotions. In severe cases, use systemic antifungal agents.
- Increasing immunity and improving local blood circulation, treating the underlying disease.
- Desensitizing therapy. Since mycosis of the feet is often accompanied by allergic reactions, antiallergic drugs are prescribed accordingly, which will help improve the patient’s condition.
Treatment at home
- To effectively treat mycosis of the feet, it is necessary to remember that fungi multiply in a moist environment. By excluding moisture, fungi will not develop, and the chances of cure will increase.
- Protect your family members from fungal diseases. You should explain to them that from now on you can’t walk barefoot in the apartment, especially in the bathroom or shower room. After taking a bath or shower, it is necessary to treat the bath itself, the tray and the floor with a disinfectant.
- Wash your feet every day with soap, collecting all the fallen pieces of skin with a napkin so that nothing gets under the nails.
- After washing your feet, be sure to dry the spaces between your toes with toilet paper or a hairdryer, and then apply an antifungal agent prescribed by your doctor. Treatment must be continued for several months even in cases where the manifestations of mycosis completely disappear.
- Use powder while wearing shoes.
- Wear white cotton socks (clean every day). Used socks should be boiled or soaked in disinfectant for 10 minutes. Shoes must be disinfected using antifungal sprays.
Prevention of mycosis of the feet
Timely treatment of diseases that can reduce the body's defenses or impair blood circulation.
Conclusion
Foot fungus is one of the most common fungal skin infections. In most cases, following simple rules of prevention helps to avoid the disease, and timely treatment begins to completely get rid of mycosis.

























